Making new friendships has been the most surprising gift from my unexpected diagnosis of Myelodysplastic Syndrome (MDS) and subsequent stem cell transplant. I’ve met many brave and inspiring people on this journey through support groups, Facebook, and word of mouth.
About a month after my transplant, I met Karen B. at an online support group. She was getting ready to have a transplant and was there to ask questions. She asked me for my email address in the chat. I gladly shared it and have enjoyed many conversations with her since.
We’ve spoken about every month over the past two years, and I asked her if I could share her story. I offered her a list of questions to respond to and got much more than anticipated. Her strength, inventiveness, and grit are inspiring.
Tell a little about yourself.
My name is Karen B. I live in Altadena, California, a little town north of Pasadena at the base of the mountains. I work for a mental health facility, where I process and track claims and insurance payments. I have a wonderful and caring family and many friends who have supported me through the process. My hobbies are crocheting and cooking, and after dinner, I enjoy sitting down and watching a couple of hours of TV.
Would you share your diagnosis?
July 2021: I had routine blood work completed after my annual physical (missed 2020 physical due to COVID). My doctor contacted me and told me that there were abnormalities and that I needed to go to a Hematologist/ Oncologist. I said I felt fine and to rerun the tests, and if there were a problem, I would go. Well, the second set returned a tad worse, so I met with a Hematologist/ Oncologist, had more blood work, and then a bone marrow biopsy (BMB) in December 2021. On January 3rd, 2022, I received the call that would change me.
I had Myelodysplastic Syndrome, MDS. I went for three-second opinions and chose Dr. Ryotaro Nakamura at the City of Hope, A Cancer Center of Excellence. My initial diagnosis was moderate leukopenia/thrombocytopenia and ~7% blasts, normal cytogenetics, and BCOR and STAG2 mutations. Hypocellular marrow (25%) with dysplastic changes and 5% blasts by morphology, 7.6% by flow, c/w MDS-EB1. Neg GMS, PAS, TB IHC. That’s a mouthful, isn’t it?
What did you feel at the time of your diagnosis, and what actions did you take?
First, I thought this couldn’t be happening. You tell your family and friends and feel like this story is not yours but someone else’s. I cried and cried and then cried some more. I was not happy. My mom always told me to try to think of the worst outcome whenever I had to accomplish something hard. Then, maybe, I’d find out it’s probably not as bad as I’m making it out to be. So, I tried to follow her advice.
The problem was my worst outcome was death. Well, I was raised and am a practicing Catholic. So what was I scared of? I wanted to see my friends and family and didn’t want to leave them, but if God had other plans for me, who am I to question him? From that point on, I was more relaxed and understood the process.
Plato said, “Death is not the worst thing that can happen to a man.” Once I stopped being afraid of death, it was easier for me to fully understand what I needed to do. I stopped spending time being upset. I changed my attitude right around the second time my information was run through the database (Be The Match), and a match was found. When my doctor said the tests went well to confirm the match, I started prepping for my transplant.
Octavia Spencer said, “You have to think a little smarter, be proactive, not reactive. The way to bring about change is to be proactive and active.” “Regret is not a proactive feeling” became my new mantra. Between that and my positive attitude, I knew I could do this.
I’m great at writing and following lists. Here are a few items from a list of things I did to prepare for my transplant experience:
· Financial accounts and monthly bills with payment due dates for my husband.
· Write goodbye letters to my children, my husband, and a couple of friends.
· What I needed to take with me to be able to work from the hospital.
· Email friends and relatives to send me photos to upload to my picture frame.
· Talk to HR and Supervisor to go over expectations.
· Prep freezer meals for while I'm in the hospital.
· A weekly washing list: Monday, wash bedsheets; Tuesday, wash bath towels; Wednesday, wash kitchen towels; Thursday, wash cleaning rags
This is just a sampling. The entire list was two pages long. It made me feel in control to create these lists.
What was the donor search like?
The first time, my information was run through the Be The Match database, and there wasn't a match among the over 30 million people registered. Talk about depressing.
My family produced fliers and handed them out EVERYWHERE to ask people to get on the Be The Match database. All it requires is a swab of the cheek. Facebook, Instagram, and Twitter all had posts asking people to consider swabbing. Once a match based on the initial swab is made, the donor goes through additional testing to confirm they're a match and they're healthy enough for the donation. The actual donation is like giving blood. The only difference is that the donor is given medication to stimulate the marrow and increase the production of stem cells, while the actual stem cell donation is taken from a vein in the arm by a special apheresis machine. It takes a little longer than a regular blood donation, and they try to collect enough for a few transplants if the patient needs it.
After I had another round of chemo, they ran my profile through the database again and came up with a 9/10 match, a 24-year-old male in Europe. Hooray!
And that was just the beginning. Now, I had to go through the process of screening to see if I was healthy enough to withstand the transplant. Meanwhile, somewhere in Europe, this man who would save my life was going through his own set of tests to see if he was healthy enough to donate. In case you're curious, here's how a donor is matched. The best marrow transplant outcomes happen when a patient's human leukocyte antigen (HLA) and the HLA of a registry member or cord blood unit closely match; currently, they use 12 markers. A perfect match is when you have a 12 out of 12 match. In 2022, they tracked 10 markers. I had a 9 out of 10 match.
Describe your transplant experience.
Pre-transplant conditioning started as soon as I was admitted. I was on a heavy-duty chemotherapy regime for 6 days, then a two-day break right before the transplant, and 1 additional heavy-duty chemotherapy three days after the transplant. There was no radiation involved. Regimen: IRB 21216 was the exact regime with Fludarabine/Melphalan/Cyclophosphamide/Tacrolimus/Mycophenolate Mofetil (Cryo-PBSC).
My transplant was scheduled for 6/13/2022 at City of Hope, which is a Cancer Center of Excellence in Duarte, California. I’d already been there for a few days and was used to the nurses’ routine. I wasn't able to get either an exact time or timeframe for the transplant. So, I took the entire day off work, which was the waiting game. My husband came in the morning to wait with me. We watched TV, FaceTimed with friends and family, and waited. Hurry up and wait isn't my favorite thing to do.
When the transplant nurse and scientist finally arrived, I was more than ready. My husband was really interested in the actual procedure, and I just wanted to get it over and done. I told everyone I would “go to my happy place - so don't bother me.” I turned on my left side, closed my eyes, and breathed. The nurse had hot pads, oxygen, and smelling salts available. The transplant cells were frozen; they were placed into hot water for a short time and then hung and processed through my IV; multiple bags of cells were used, and the entire process took from 11:30 am to 5:53 pm. It was anticlimactic. I didn't feel any different - just very tired and worn out.

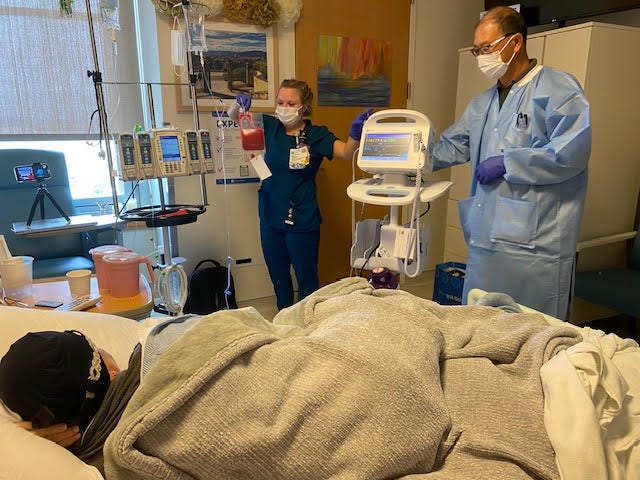
While I was in the hospital after the transplant, I received daily transfusions of either platelets, whole blood, or sometimes both. I had fevers, stomach pain, and a lack of energy. Three times a day, my nurses would provide me with a “cocktail,” which helped me with the pain and nausea. My energy level eventually returned as I pushed myself to do more physical activity.
My day started at midnight. The nurses would come in and take blood for testing. My results would come in at 2 am, and I would find out what transfusions I needed. (Side note: Because my family had set up a Direct Blood and Platelet Donation schedule—Seventy-five constant donors for both whole blood and platelets—I didn't have the problem some patients have with not having enough blood in the blood bank.)
Once the results were in, I would ask for my transfusions to start in enough time for me to complete them so that I could start work at 9 am. Both whole blood and platelet transfusions can last up to 3 hours each and require premedication, which allows you to have the transfusions without side effects of chills, vomiting, tachycardia, and hypertension. Since I was both whole blood and platelet dependent, some mornings, my transfusions would last until anywhere from 5 am to 8 am. After the transfusion, I would get dressed, wrap my head, and brush my teeth. I'd have breakfast at around 8:30 and be ready to go to my Zoom area to start work at 9 am. Doctors would take their rounds between 10-11:30 am.
To prepare for me to be able to work during my hospital stay, my daughter and her roommate cut up five shirts along the side and put snaps so that I could get dressed and not have to wear a hospital gown to work. My daughters and husband decorated my room and set up a special Zoom area. I would work until about 2 pm, eat lunch, take a nap, and then have physical therapy.
I’d like to thank my wonderful employer, The Camden Center, for allowing me the flexibility to continue working while I was in the hospital. Maintaining my daily schedule was a big part of helping me recover.
What was your total time in the hospital?
The doctors initially thought I would be in the hospital for 30 days, 4 days pre-transplant and 26 days post-transplant. Because of good test results and my strong desire to get out of the hospital as soon as I could, that changed to a total of 21 days: 4 days pre-transplant and 17 days post-transplant. Two days of my infusions were done outpatient. The doctor put me into the hospital earlier than they normally do because my daughter's graduation was that weekend (6 hours away from our home). My doctor and husband didn't want me to be home alone.
What was your life like after you were released from the hospital?
Because I live close to the City of Hope, I was able to go directly home after my husband and daughters received training on how to take care of me.
In preparation, my family had to undergo three hours of training. Here, they learned the importance of constantly disinfecting everything I could come in contact with. Air purifiers need to be placed in every room, bedsheets, and bath towels had to be changed daily after being washed in hot water with bleach, underwear had to be washed separately, and dishes, glasses, and utensils had to be washed with antibacterial dish soap and hot water.
For about three months, I went to City of Hope three times a week for bloodwork, follow-up doctor appointments, and an occasional IVIG infusion. After that, my appointments dropped to two times a week, then once a week, then every other week, then once a month. At eighteen months post-transplant, I was dropped to once every six weeks.
After a stem cell transplant, you lose ALL of your immunities. All of your vaccines from when you were a baby need to be repeated, but those can’t start until eighteen months post-transplant. For the first year, your immunity is like a baby's. I am still on Mepron (an immunosuppressant) and Acyclovir (an antiviral) and occasionally have an IVIG infusion to increase my immunoglobulin.
What did your initial post-transplant test results look like?
They were on the low side of normal for most everything. WBC, Hematocrit, Platelets, Neutrophils, Monocytes, RBC, Hemoglobin etc... But they were all normal, normal, and more normal. Yay!
After my first hundred days, the bone marrow biopsy showed that my donor cells made up over 90% of my blood—in fact, the numbers were in the high 90s.
All tests showed that my MDS was put in remission because the diseased cells were gone.
What kinds of things did you experience after the transplant?
My hair was always important to me. Because I didn't have much control over my hair, when my doctor told me I would lose it all from the chemo, I decided how and when to let go of it. So I invited family and some friends over and had a Buzzzzzz Party. My daughter put my hair into about 20 ponytails, and then everyone who came had a chance to cut a ponytail or two. After my hair had been cut, a friend of mine who's a comedian came over and gave me the final shave while doing a comedy routine. Once I was in the hospital, my hair, what little there was, started to fall out, and I kept breathing it in. I eventually had the hairstylist that the City of Hope keeps on staff come and shave my head again. Afterward, I kept a lint roller at my bedside to roll over my scalp.
Six months later, on Christmas Day 2022, I felt comfortable removing my head covering when I was in public. A year later, on Christmas Day 2023, I was back to blow drying and flat ironing my hair, which is now close to its length before this ordeal.
My doctors said I could eat anything I felt comfortable eating. After the transplant, there were some restrictions. No raw or rare food. Sushi and Sashimi I don't like, but getting used to a well-done steak, yuk. There's a Mediterranean meal that's meat mixed with bulgar and spices, which I absolutely love. That was out. All fruits and vegetables had to be washed in a special produce wash to clean them, and they all had to be cooked if they couldn't be peeled. No cutting up an orange or apple at the table after dinner or having a slice of melon for dessert. Freshly squeezed juices were out, too; everything had to be pasteurized. Lunch meats were out.
All food had to be made at home, so there was no going out for a meal or having takeout. It was very important that cleanliness and cooking standards were met, and there was no guarantee that this would happen without making it yourself. My husband found a "cheat.” My hospital, City of Hope, has a full-service hotel attached to it. There, they have a restaurant that meets the standards, outdoor seating, and great food.
While I was in the hospital, I had to measure and track both urine and feces. Amount? Color? Texture? It was like diamonds: Color, Cut, and Clarity. The nurse brought me a flashlight so that I could see inside the toilet and give a more accurate description.
When I got home, nausea would come out of nowhere. I kept those green "barf bags" throughout the house wherever I normally sit. Between diarrhea and constipation, it was a toss-up; each day was different. I never knew what was going to come out.
Graft vs. Host Disease (GVHD) showed up on my skin and progressed all over my body. In my second month, the doctors tried to switch my immunosuppressant medication from Mepron to something more tolerable. Mepron tastes horrible. When they switched me to another medicine, it triggered my skin GVHD to get worse. A one point I had blotches from the top of my head to my toes. After switching back to Mepron, they also increased my prednisone dosage and added a tacrolimus cream (another type of immunosuppressant) to help reduce my GVHD. Recovery took around a month. I still sporadically get flare-ups, and I have to increase oral tacrolimus and use the cream on the site of breakouts. My oral tacrolimus dosage has been tapered to two .05 mg doses in the morning and two in the evening. That's down from 100 mg a day.
What was the most difficult thing about having a stem cell transplant?
I couldn't be with my family and friends. For the first year, I had to stay away from everything and everyone. I couldn't get sick and wasn't sure how I would react.
Thank God for Facetime and ZOOM
How has this experience changed you?
The expectation of the transplant being a success was not in my favor. My doctor said while the match wasn't perfect, it was “a good shot.” This is why I take each day as an experience I may not have had a year and a half ago. I look at my life with “fresh eyes.”
Without the transplant, I would die.
With the transplant, I had a chance to live.
If you had to do it again, would you?
I would do it again, but I had no other options.
Anything else you'd like to share?
MDS is a disease that, if not caught early enough, can mushroom into Acute Myeloid Leukemia (AML). If it's caught early, you can be on a watch and wait. If it's too late, then it's morphed into AML, and the treatment is much more difficult.
Here are a few suggestions for anyone who gets a diagnosis like this:
Make sure to go to a Cancer Center for Excellence.
Use the resources available to you: social workers, insurance company transplant department,
When people reach out to help, say YES – can you make dinner one night, go for a walk with me so I'm not walking by myself (if you feel uncomfortable – wear a mask)
Do as much as you feel you can do. I worked remotely from the time I was diagnosed through treatment and during the entire time that I was in the hospital. I kept a schedule and stuck to it.
Be Proactive, not Reactive. Set up a direct Blood and Platelet Donation for friends and family.
If you're in the hospital for an extended stay, make the room yours. Put up banners, posters, and anything that will make you smile. Remember, most transplant rooms won't allow flowers or plants, but streamers and balloons should be ok.
Zoom and Facetime are your friends. Hook up to the Wi-Fi and visit with family and friends.
Keep a calendar so that you can track things and not have to rely on your memory. Chemo Brain is a real thing. Crossword puzzles, WORDLE, really anything to keep your mind going.

Karen B. is amazing, isn’t she?
I highly recommend that anyone who gets a troubling and life-threatening diagnosis find a support group as soon as possible. Being part of these groups has helped me in so many ways. We laugh, we cry, we share strategies, and, most of all, we support each other. I now lead a Transplant for MDS support group through AAMDS. We meet once a month, and the members range from long-term “thrivers” to individuals still unsure about having a transplant.
For more information, here's a list of websites:
Be The Match - now called - National Marrow Donor Program







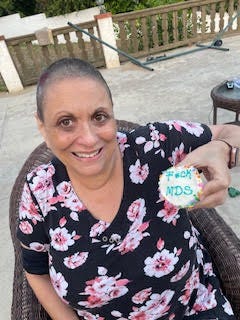

Beautiful expression of Attitude from true Faith.
This is both so good and so interesting. I’m happy to know about the donor program. Many thanks to you both.